Would be grateful for any advice.
I currently have the following symptoms: unusual gum tenderness, rapid and recent recession of the gum in the same area, odd taste in mouth, discomfort (sensation of gum compression) that wakes me up at night. I have seen two dentists and an endodontist in the last two weeks, none of whom have diagnosed any problem needing treatment. I am concerned that they are missing something (decay under the crown?) as I do not feel the symptoms I am experiencing are psychosomatic. I am posting here for advice as I'm concerned enough to be considering asking to have the crown removed on my own recognizance, I recognise this might risk killing the tooth.
The symptoms are around a ten year old PFM crown on a molar (live tooth that I think weakened due to poor brushing discipline and cracked on top after biting on something hard). It has had a large gap with the adjacent tooth for a while but this has been OK for years with active tooth cleaning after meals. Nowadays my brushing and flossing discipline is good and dentists comment on this at the annual checkups. I have a full set of teeth otherwise, no recent cavities although many old ones.
About a month ago I got a seed stuck under this adjacent tooth and did not realize it for several days (floss and pick didn't get it out, interdental brush finally did). I had bad inflammation around the area and gum tenderness. This kind of thing has happened before but never as long and the symptoms have never been as bad. I started to find I had a metallic taste in my mouth on that side and the gum was painful. The gap between the teeth felt larger. Swishing mouthwash there feels uncomfortable. There is tenderness and discomfort around the gums in the area. Chewing is not painful.
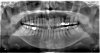
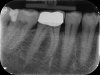
Dental x-rays show no decay although the dentists caveat that they can't see decay if it is in the crown. The endodontist saw no sign of infection and suspects instead trauma from too vigorous teeth cleaning with picks and floss. A few days of being more gentle in cleaning has not changed anything. She did point out that the interdental papilla between the crown and the other tooth has disappeared - no dentist has pointed this out before and it matches my feeling that the space has recently become larger.
I feel out of options to address this issue, I am doing very occasional salt rinses, brushing gently with fluoride three times a day, and applying chlorhexidine digluconate as both the dentists advised. If the symptoms persist more than another week or two I strongly feel I will have no choice but to ask them to drill off the crown and see what is under there (would replacing it with gold be a stupid idea now that the tooth has been filed down for PFM? Dentists in my area, perhaps any area nowadays, don't seem to even consider gold, which I think is how I got the PFM crown to begin with.)
As I said, grateful for any advice. Frustrated that the dentists I have seen don't see my symptoms as a problem (or perhaps view it as likely to self resolve). How long would you wait to do something?
I currently have the following symptoms: unusual gum tenderness, rapid and recent recession of the gum in the same area, odd taste in mouth, discomfort (sensation of gum compression) that wakes me up at night. I have seen two dentists and an endodontist in the last two weeks, none of whom have diagnosed any problem needing treatment. I am concerned that they are missing something (decay under the crown?) as I do not feel the symptoms I am experiencing are psychosomatic. I am posting here for advice as I'm concerned enough to be considering asking to have the crown removed on my own recognizance, I recognise this might risk killing the tooth.
The symptoms are around a ten year old PFM crown on a molar (live tooth that I think weakened due to poor brushing discipline and cracked on top after biting on something hard). It has had a large gap with the adjacent tooth for a while but this has been OK for years with active tooth cleaning after meals. Nowadays my brushing and flossing discipline is good and dentists comment on this at the annual checkups. I have a full set of teeth otherwise, no recent cavities although many old ones.
About a month ago I got a seed stuck under this adjacent tooth and did not realize it for several days (floss and pick didn't get it out, interdental brush finally did). I had bad inflammation around the area and gum tenderness. This kind of thing has happened before but never as long and the symptoms have never been as bad. I started to find I had a metallic taste in my mouth on that side and the gum was painful. The gap between the teeth felt larger. Swishing mouthwash there feels uncomfortable. There is tenderness and discomfort around the gums in the area. Chewing is not painful.
Dental x-rays show no decay although the dentists caveat that they can't see decay if it is in the crown. The endodontist saw no sign of infection and suspects instead trauma from too vigorous teeth cleaning with picks and floss. A few days of being more gentle in cleaning has not changed anything. She did point out that the interdental papilla between the crown and the other tooth has disappeared - no dentist has pointed this out before and it matches my feeling that the space has recently become larger.
I feel out of options to address this issue, I am doing very occasional salt rinses, brushing gently with fluoride three times a day, and applying chlorhexidine digluconate as both the dentists advised. If the symptoms persist more than another week or two I strongly feel I will have no choice but to ask them to drill off the crown and see what is under there (would replacing it with gold be a stupid idea now that the tooth has been filed down for PFM? Dentists in my area, perhaps any area nowadays, don't seem to even consider gold, which I think is how I got the PFM crown to begin with.)
As I said, grateful for any advice. Frustrated that the dentists I have seen don't see my symptoms as a problem (or perhaps view it as likely to self resolve). How long would you wait to do something?
Last edited: