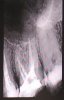
Three months back, as a very old and large filling in my maxillary second molar (upper left tooth #7) had broken and developed a gap between the filling and tooth (as per what the dentist told me), I was advised to get it replaced. Otherwise the tooth was completely asymptomatic and very solid. As I really wanted to avoid a root canal down the road, I agreed. However, the dentist kept drilling for a long time. I asked if it was really necessary (as I had just gone to get a filling replaced and obviously wanted to avoid a root canal). He said there was a lot of decay under the filling. Anyway, finally he stopped drilling and then touched the cavity with an instrument which gave me great pain. He said there was no bleeding but a root canal was the only option now. However, as I had developed some doubts and wanted to take a second opinion, I asked for time to think and he put a temporary filling in.
Now I had great sensitivity to cold and also pain when pressing that tooth from the side only (no pain from pressing from underneath). These became less in intensity after some time but remained to a minor extent.
Meanwhile, because of an ongoing (and still not resolved) more serious issue with another tooth, and failure to find a good dentist whom I could trust (as I knew that just removing the temp filling could expose the pulp), I could not get this tooth treated.
Finally, two days back, a found a dentist who said that he would try to avoid a root canal, i.e., if he could remove the temp filling without exposing the pulp, he would put an indirect pulp cap on it, but if he exposed the pulp, he would put a direct pulp cap on it. I gave him the go ahead. He said either MTA or Dycal could be used but the cost of the MTA he quoted was just too high, so I had to go with Dycal.
He said he would need to remove the temp filling to visually check the cavity, and would do so ultrasonically to avoid further destruction. However, as it was already close to the pulp, during the removal, a small pinpoint of the pulp got exposed due to mechanical trauma (he said there was no caries there). He immediately treated the exposed pulp with a laser, then he said he put formaldehyde on it (later he specified formocresol), and then he left a cotton pellet soaked in chlorhexidine on it for about a minute. After this, he put Dycal (calcium hydroxide) on it, and then covered it with a temp filling. He told me to come back after two weeks to assess my condition. If it seems to be healing ok, he would remove the temp filling (but leave around 1mm of the temp filling in place so as not to disturb the underlying Dycal) then do the permanent filling. If it's not ok, then he could do a root canal.
My questions are:
1. I read that dentin bridge formation takes time and usually the tooth should not be disturbed for anywhere from 4-8 weeks at least. Is it advisable to re-enter that tooth in 2 weeks, or how long should I ask him to wait? I am not chewing on that side at all (because of another problematic tooth) so the temp filling will not get compromised.
2. Is it ok to not remove the temp filling fully i.e. leaving 1 mm behind (on top of the Dycal) and do the permanent filling on top of it (in terms of bonding ability, long term prognosis). what precautions to take?
3. i read that calcium hydroxide gets absorbed and becomes soft and leaves a void there ultimately. Will this be a problem and can it be prevented? What precautions to take?
4. I had great pain (specifically at the pulp exposure point) right when the pulp got exposed and then after the treatment. There was great pain while pressing my tooth from the side (but not from the bottom). This was two days back. The dentist said it was due to the pulp getting irritated. Yesterday morning, the pain on all counts went down 50%. But then yesterday night, I felt some minor swelling/soreness/tenderness inside at a point which was 1 inch to the left of my left nostril. That swelling went down by this morning. However, again tonight, the minor swelling/soreness/tenderness has come back at that same point. What could it be due to? Is it normal? Will it get better? Or does it indicate any failure? Otherwise, the pulp exposure point has not gotten any worse or better yet.
5. How much time should be given to assess whether the direct pulp cap has worked or not ( at least for the time being). And how to assess it? Should the tooth be completely asymptomatic, or is some sensitivity still normal and considered successful? Because I don't want to pay for a permanent filling if I have to end up getting a root canal done very soon afterwards.
Now I had great sensitivity to cold and also pain when pressing that tooth from the side only (no pain from pressing from underneath). These became less in intensity after some time but remained to a minor extent.
Meanwhile, because of an ongoing (and still not resolved) more serious issue with another tooth, and failure to find a good dentist whom I could trust (as I knew that just removing the temp filling could expose the pulp), I could not get this tooth treated.
Finally, two days back, a found a dentist who said that he would try to avoid a root canal, i.e., if he could remove the temp filling without exposing the pulp, he would put an indirect pulp cap on it, but if he exposed the pulp, he would put a direct pulp cap on it. I gave him the go ahead. He said either MTA or Dycal could be used but the cost of the MTA he quoted was just too high, so I had to go with Dycal.
He said he would need to remove the temp filling to visually check the cavity, and would do so ultrasonically to avoid further destruction. However, as it was already close to the pulp, during the removal, a small pinpoint of the pulp got exposed due to mechanical trauma (he said there was no caries there). He immediately treated the exposed pulp with a laser, then he said he put formaldehyde on it (later he specified formocresol), and then he left a cotton pellet soaked in chlorhexidine on it for about a minute. After this, he put Dycal (calcium hydroxide) on it, and then covered it with a temp filling. He told me to come back after two weeks to assess my condition. If it seems to be healing ok, he would remove the temp filling (but leave around 1mm of the temp filling in place so as not to disturb the underlying Dycal) then do the permanent filling. If it's not ok, then he could do a root canal.
My questions are:
1. I read that dentin bridge formation takes time and usually the tooth should not be disturbed for anywhere from 4-8 weeks at least. Is it advisable to re-enter that tooth in 2 weeks, or how long should I ask him to wait? I am not chewing on that side at all (because of another problematic tooth) so the temp filling will not get compromised.
2. Is it ok to not remove the temp filling fully i.e. leaving 1 mm behind (on top of the Dycal) and do the permanent filling on top of it (in terms of bonding ability, long term prognosis). what precautions to take?
3. i read that calcium hydroxide gets absorbed and becomes soft and leaves a void there ultimately. Will this be a problem and can it be prevented? What precautions to take?
4. I had great pain (specifically at the pulp exposure point) right when the pulp got exposed and then after the treatment. There was great pain while pressing my tooth from the side (but not from the bottom). This was two days back. The dentist said it was due to the pulp getting irritated. Yesterday morning, the pain on all counts went down 50%. But then yesterday night, I felt some minor swelling/soreness/tenderness inside at a point which was 1 inch to the left of my left nostril. That swelling went down by this morning. However, again tonight, the minor swelling/soreness/tenderness has come back at that same point. What could it be due to? Is it normal? Will it get better? Or does it indicate any failure? Otherwise, the pulp exposure point has not gotten any worse or better yet.
5. How much time should be given to assess whether the direct pulp cap has worked or not ( at least for the time being). And how to assess it? Should the tooth be completely asymptomatic, or is some sensitivity still normal and considered successful? Because I don't want to pay for a permanent filling if I have to end up getting a root canal done very soon afterwards.